3 Ways to Cope With Fear of Giving Birth After a Traumatic First Birth
Fear of giving birth after a traumatic first birth is one of the most common and least talked-about experiences in pregnancy. Three evidence-based ways to cope: focus on the facts of your current pregnancy, use a rings of control exercise to separate what you can and can't influence, and identify specifically what your fear is connected to. If the fear is constant, overwhelming, or connected to flashbacks from your previous birth, trauma-focused therapy is likely what you need.
⏱️ Read time: 6 minutes — or jump to what you need most:
The thoughts that keep you up at night.
What if the same thing happens again?
What if I end up being induced and it all goes wrong?
What if the baby gets stuck?
What if something happens to me, or to the baby?
What if I make the wrong decision about how to give birth — and I have to live with that?
If these are the thoughts running through your head at 2am, you're not alone. And you're not being dramatic. You're pregnant after a birth that frightened you — and your brain is doing exactly what frightened brains do. It's trying to protect you by running through every possible thing that could go wrong, hoping that if it thinks hard enough, it can prevent it.
It can't, of course. But knowing that doesn't make the thoughts stop.
This article won't promise to take the fear away. But it will give you three things you can actually do — right now, before any therapy appointment or consultant meeting — that genuinely help.
Why This Decision Feels So Hard
You're Not Alone — And This Is More Common Than You Think
You are not the only one feeling this way. Not even close.
Around 30,000 women a year in the UK experience birth trauma — and most of them receive no trauma-specific support at all. Research shows that between 3–6% develop full PTSD after childbirth (Ayers, 2017) — but that's just the tip of it. Many more are living with flashbacks, panic before appointments, and a constant low-level dread that something will go wrong again. Symptoms that don't just fade when a new pregnancy starts. Often they get louder.
Up to 14% of pregnant women experience tokophobia — a clinical level of fear of childbirth — and secondary tokophobia, which develops after a traumatic first birth, is actually more common than fear in women who have never given birth before (O'Connell et al., 2017).
So if you're sitting here, bump growing, absolutely dreading what's coming — you're not broken. You're not weak. You had a frightening experience, and your body and mind haven't forgotten it. That's not a flaw. That's how humans work.
And it deserves more than someone telling you to think positive.
Why Your Fear Makes Complete Sense
Here's what's actually happening when the fear hits.
Your brain went through something frightening the first time. Maybe you felt out of control. Maybe people didn't listen. Maybe something went wrong that you weren't prepared for, or your body did something you didn't expect, or you came away feeling violated or guilty or completely alone in it. Whatever it was — your brain filed it. Stored it. Labelled it: dangerous.
And now you're pregnant again, and your brain is doing exactly what it's supposed to do with dangerous things. It's scanning. Watching. Running through every possible version of how this could go wrong again.
The problem is your brain can't tell the difference between remembering something terrifying and actually being in danger right now. So the fear feels immediate. Real. Present. Not like a memory — like a threat.
That's not you being unable to cope. That's not weakness. That's your nervous system doing its job — just in a situation where the job has become exhausting and overwhelming.
And it can get better. That's the part most people don't tell you.
3 Ways to Cope With Fear of Giving Birth Right Now
These aren't cures. They won't process the trauma or take the fear away completely. But they will help you feel less overwhelmed — and sometimes that's exactly what you need to get through the next few days or weeks while you work out what proper support looks like for you.
1. Come Back to the Facts of This Pregnancy
When the fear takes over, it stops being about this pregnancy. It becomes about every pregnancy. Every worst case. Every version of what could go wrong. Your brain stops processing what's actually happening right now and starts catastrophising about what might.
So bring it back. Just to this pregnancy. Just to right now.
Ask yourself: what has my care team actually told me about this pregnancy? Is it low risk or high risk? What did the 12-week and 20-week scans show? What has my midwife or consultant said about my options? What do I actually know — as opposed to what I'm afraid might happen?
This isn't about pretending everything is fine. It's not toxic positivity. It's about noticing the difference between what is actually happening in your pregnancy right now — and what your frightened brain is generating on top of it. Fear is incredibly good at making imagined dangers feel just as real as actual ones. Facts are one of the few things that can interrupt that spiral.
If you genuinely don't know the answers to some of these questions — that's useful information too. It might mean there are specific conversations to have with your care team that would help you feel more grounded. You're allowed to ask. You're allowed to say "I had a traumatic first birth and I need more information to feel safe in this pregnancy." A good midwife will respond to that.
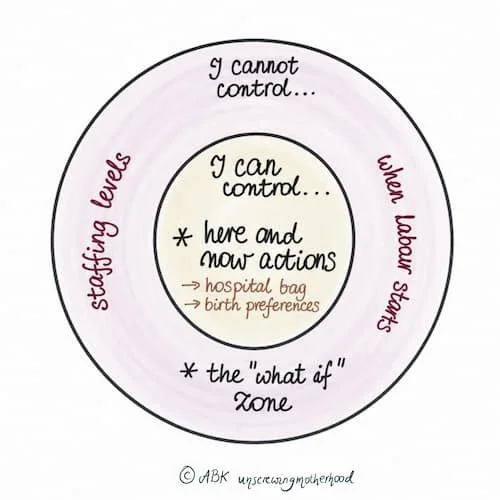
2. Use Rings of Control
One of the cruelest things about birth fear is this: you cannot control the outcome. You know that. And for someone who has already been through a birth that went differently from what she hoped — that knowledge is terrifying.
You can't fix that. You can't make birth predictable. But what you can do is get very clear on what is actually within your reach — and put your energy there instead of burning it on the things that aren't.
That's what this exercise does.
Draw two circles — a small one inside a larger one. In the outer ring, write everything you cannot control: when labour starts, whether the birthing pool is free, staffing levels on the day, whether complications arise, what your baby decides to do. These are real and valid fears. And they are outside your control.
In the inner ring, write everything you can influence: writing a birth preferences plan that clearly communicates what you need, packing your hospital bag so you feel prepared, choosing who will be with you and briefing them on how to advocate for you, eating well and resting, knowing who to call and what your options are if labour starts unexpectedly, making sure your care team knows your history.
The inner ring is where your energy belongs. Not because the outer ring doesn't matter — it does. But because spending all your energy trying to control the uncontrollable is exhausting and it doesn't work. Focusing on what you can do gives your nervous system something useful to do with the fear.
3. Look Honestly at What You're Actually Afraid Of
Not all birth fear is the same — and understanding what's specifically driving yours is one of the most useful things you can do.
Get a piece of paper and write down every specific fear you have about this birth. Don't filter it. Write it all down.
Then look at what you've written and ask yourself: are these fears about the unknown — things that might happen that you have no way of predicting? Or are they connected to something specific that happened last time — not being listened to, not feeling safe, feeling out of control, feeling violated or dismissed or alone?
If your fears are mostly connected to specific things that happened in your previous birth, that's important information. It means there are concrete things that can be addressed. A birth preferences plan written with those specific fears in mind — one that directly asks your care team to do things differently this time — can make a real difference. Talking to your midwife or consultant about what happened and what you need can shift things significantly. I've written about how to approach that conversation here.
If your fears are more about general catastrophising — the "what ifs" that spiral endlessly — that's a different kind of work, and the first two steps above will help more.
And if when you look at your list you realise that the fear is overwhelming, constant, affecting your daily life, or connected to flashbacks and intrusive memories from your previous birth — that's a sign that what you're experiencing goes beyond birth anxiety. That's birth trauma. And birth trauma needs processing, not just managing. You can read more about what birth trauma is and how it's treated here: [link to birth trauma blog].
When Coping Isn't Enough
These three steps are real and they help. But they have a ceiling.
If you've tried them and the fear is still overwhelming — if it's waking you up at night, making you dread appointments, affecting your relationship, making it impossible to feel anything about this pregnancy except terror — that's not a coping problem. That's trauma. And trauma needs more than coping strategies.
It needs processing.
Trauma-focused CBT and EMDR therapy — both recommended by NICE — work differently from talking therapy or counselling. They don't just help you manage the fear. They work on the actual memories and meanings from your previous birth that are keeping the fear alive. The moment in labour when you lost trust. The thing someone said. The feeling of not being in control of your own body.
Once those are processed — really processed, not just talked about — things shift. I see it regularly with the women I work with. The fear doesn't vanish. But it stops being the thing that's running every decision you make about this pregnancy.
If you're also trying to work out whether to request a C-section this time, I've written specifically about that here — including what NICE guidelines actually say and what the decision is really about:
One More Thing...
If you've got to the bottom of this article and something in it has felt uncomfortably familiar — that recognition is worth paying attention to.
You can book a free 20-minute conversation below. It's not a sales call. It's a chance to talk about what's been hardest, what you most want to feel differently, and whether the way I work sounds right for you. No pressure and no obligation.
Not ready for a call yet? Email me instead — just a few lines about where you are. We can go from there at whatever pace feels manageable. There's no wrong way to start.
Sessions are £130 • Online across UK, EU and internationally • Weekly sessions available
Hi, I’m Aleksandra!
A BABCP-accredited CBT therapist specialising in perinatal trauma, birth trauma, and tokophobia. I have supported women with birth trauma and fear of childbirth for over ten years, working within NHS perinatal mental health services and in specialist private practice. I am completing EMDR training through EMDR Academy in May 2026.
I work online with women across the UK, EU and internationally. I combine trauma-focused CBT with EMDR therapy and compassion-focused approaches — and I'll work with you to find what actually helps, not just what's supposed to help in theory.
FAQs: Fear of Giving Birth After Traumatic First Birth
-
Yes — completely. Research shows that trauma symptoms following childbirth are far more common than most people realise, and fear of a subsequent birth is one of the most consistent responses. Your fear isn't irrational or dramatic. It's your nervous system doing exactly what it learned to do after something genuinely frightening. The question isn't whether the fear makes sense — it does — but whether it's so overwhelming that it needs more than coping strategies to address.
-
For some women, fear eases as they feel more prepared and as the pregnancy progresses well. For others — particularly those experiencing trauma symptoms connected to their previous birth — fear tends to increase as the due date approaches rather than ease. If your fear is getting worse rather than better, that's a signal it needs proper support rather than time.
-
This is one of the most common questions — and the guilt it carries makes the anxiety worse. Normal pregnancy anxiety, even when intense, is unlikely to harm your baby. However if your fear is preventing you from attending antenatal appointments, affecting your ability to eat or sleep, or causing severe panic responses, it's worth seeking support — not because you're harming your baby, but because you deserve to feel better. Your wellbeing matters too.
-
Birth anxiety is fear about the upcoming birth — worry about pain, complications, loss of control. Birth trauma is the psychological aftermath of a previous birth experience that felt threatening, frightening, or violating — and it often drives the anxiety in subsequent pregnancies. If you're having flashbacks, intrusive memories, or panic responses connected to your previous birth, that's trauma rather than anxiety, and it needs a different kind of support. You can read more about birth trauma here: [link to birth trauma blog].
-
You don't have to find the perfect words. You can simply say: "My last birth was traumatic and I'm finding it very hard to feel safe about this one. I need more support." A good midwife will take that seriously, ask questions, and work with you on a plan. If they dismiss your concerns, you are allowed to ask for a different midwife or a referral to a perinatal mental health specialist. You don't have to manage this alone within your care team.
-
If the fear is affecting your daily life, your sleep, your relationships, or your ability to engage with this pregnancy — seek support now. You don't have to wait until things are at crisis point. Trauma-focused therapy before your due date gives you the most time to process what happened and prepare for this birth differently. Earlier is almost always better.
Let’s connect:Disclaimer:
The information provided in this article is for educational and informational purposes only. It is not intended to be a substitute for professional medical or mental health advice, diagnosis, or treatment. Always seek the guidance of your healthcare provider, mental health professional, or other qualified health provider with any questions you may have regarding your pregnancy or mental health.